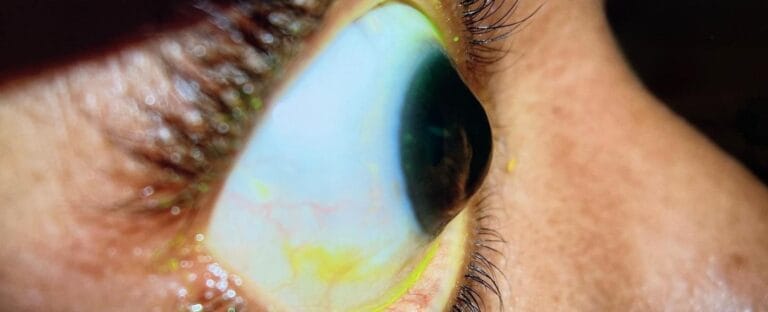
What is Keratoconus
Keratoconus is a progressive bilateral thinning of the cornea. The cornea starts to progress to a cone shape over time from the original spherical shape. Early signs start occurring in adolescence, as thinning occurs then the vision starts to decrease. There is a genetic component associated with the diagnosis but it is not very well understood. Research shows that some patients have a family member with keratoconus and in some cases it is not a direct family member.
There is an association with collagen disorders such as Ehlers-Danlos or Marfans syndrome. This is likely due to the fact that keratoconus occurs with thinning of the collagen bonds in the cornea and these syndromes occur due to collagen disorders. There are cases where keratoconus is associated with allergies and asthma. This association is not as strong as collagen disorders.
Signs
Since keratoconus is slowly progressive, it is only noticeable once it’s more severe. At first, vision will be blurry and glasses will be needed to correct vision. With time, glasses will not be enough for good vision at which point contacts will be needed.
Keratoconus is seen with patients with irregular corneas, high astigmatism and high prescriptions. Patients will present with thin corneas, overtime they can present with vertical lines (Vogt strie), scissoring reflex on retinoscopy and irregular mires in keratometry. Later signs include hydrops where the thinning leads to edema which results from a tear in a layer of the cornea.
An eye exam by a healthcare professional is highly recommended for diagnosis.
Management
There is no cure for keratoconus, but the condition can be managed. There are different treatment options for patients with keratoconus. Mainly contact lenses are recommended as these change the optics of the cornea and optimize vision. There are different types of contact lenses that differ by materials and also how the lens interacts with the eye. Practitioners will asses the cornea and its interaction with the lens. The picture below illustrates a steep cornea with a lens above it. In this image the cornea and the lens happen to be interacting, ideally there is a larger space between the lens and the cornea.Scleral lenses
Scleral lenses
are one of the best treatment options. Scleral lenses are a type of hard lens that sits on the eye. They are a larger diameter lens that sits on the white part of the eye, these does not touch the cornea which is the most sensitive part of the eye. These lenses allow for a space between the cornea and the lens which is filled with sterile saline. This space allows for optimal vision as the new lens is changing the optics of the eye. These types of lenses are durable and help with comfort and other issues in the eye such as dry eye.
There are different options when it comes to Scleral lenses, different companies have different materials and make lenses differently. Diameters of the lens vary, as well as how steep or flat the lenses are. Depending on each eye the fit will vary to what is optimal.
For example, smap3D technology maps the shape of the eye with a topographer that captures all the hills and valleys of the white part of the eye. Meanwhile EyePrint uses impressions to map the shape of the eye. These two options are highly customizable options for patients that have not been successful with other Scleral lenses.
Rigid Gas Permeable Lenses
These are another form of hard lenses, but unlike Scleral lenses these are smaller in diameter. They sit on the cornea portion of the eye and move with each eye blink. These lenses also change the optics of the eye by smoothing the surface which allows light refracting of the cornea to be regular. Although these lenses are adequate optics, with advanced keratoconus they tend to fall off.
Soft Contact Lenses
Soft contact lenses are helpful for patients with early keratoconus with more regular corneas. Soft lenses are not able to be made as specific to each person as Scleral and RGP lenses which means over time vision will not be as crisp. These types of lenses will also need changes in prescription more often than hard lenses. They also stick to the cornea more which does not give that new optical surface that hard lenses do give.
Corneal Collagen Crosslinking
This is a new form of management that has been shown to slow progression of keratoconus. This is more invasive than contact lenses, it uses UV light to strengthen the collagen cones in the cornea. There has been an overall good prognosis where the patient’s cornea has strengthened.
When managing keratoconus it is always important to know what options there are and what the best option available is for each patient.