7800 SW 87 AVE SUITE B-270 MIAMI, FLORIDA 33173
Contact Us
- Home
- Glaucoma
Glaucoma
Glaucoma: The Unseen Threat to Vision
Glaucoma refers to a cluster of eye conditions that, much like a thief in the night, progressively rob the eyesight. Often, there are no early warning signs or painful symptoms. Remarkably, it is projected that up to half of those impacted by glaucoma might not be aware they have it.
Decoding Glaucoma
At the core of glaucoma lies damage to the optic nerve – the “cable” composed of over a million ‘fibers’ that carries visual information from the eye to the brain. Previously, it was thought that optic nerve damage resulted mainly from high intraocular pressure (IOP), but modern medical understanding recognizes that even individuals with ‘normal’ IOP can experience vision loss due to glaucoma, suggesting the involvement of other factors.
Categories of Glaucoma
In adults, Glaucoma principally manifests as Open Angle Glaucoma and Closed Angle Glaucoma.
Primary Open Angle Glaucoma (POAG) is the most prevalent type, affecting an estimated 3 million Americans. This variant generally impacts both eyes and triggers ocular damage when the eye produces excessive fluid or its drainage canals become blocked, raising IOP. Individuals’ susceptibility to optic nerve damage can vary and change throughout the disease’s progression. If diagnosed and treated early, POAG typically responds well to medication, though the lost vision cannot be restored.
Narrow Angle or Angle Closure Glaucoma, though rarer, is characterized by a sudden increase in eye pressure. This occurs when the drainage canals become obstructed, much akin to a sink drain getting blocked. The typical treatment approach involves surgery that removes a small part of the iris’s outer edge, unblocking the drainage canals.
Normal Tension Glaucoma is a subtype where the optic nerve sustains damage despite ‘normal’ IOP. Individuals with a family history of normal tension glaucoma, people of Japanese ancestry, and those with hypertension or systemic heart disease are at higher risk. The mainstay treatment approach involves lowering IOP with medicines or surgery.
Pigment Dispersion Syndrome or Pigmentary Glaucoma is a less common variant that typically impacts younger people. It occurs when pigment granules detach from the iris and disperse into the clear fluid inside the eye, potentially obstructing the drainage canals and damaging the optic nerve.
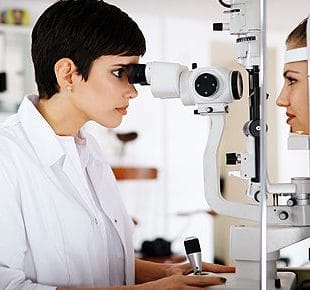
Dynamic Contour Tonometry: An In-Depth Examination
Tonometers are integral instruments used in ophthalmology to measure intraocular pressure (IOP), a critical factor in the diagnosis and management of glaucoma. For the better part of half a century, the Goldmann tonometer was considered the gold standard in IOP measurement. However, it was far from perfect.
The Shortcomings of the Goldmann Tonometer
Introduced in the 1950s, the Goldmann tonometer was recognized for its limitations. Its accuracy was optimal for corneas of a specific thickness, approximately 520 microns. Its accuracy waned as the corneal thickness deviated from this benchmark. It also did not provide reliable measurements for patients with altered corneas due to conditions such as keratoconus, or those who underwent procedures like corneal transplant surgery, LASIK, PRK, or Radial keratotomy (R-K) surgery. The flaws of the Goldmann tonometer became glaringly evident during the Ocular Hypertensive Treatment Study (OHTS) and have been discussed extensively in contemporary ophthalmic publications.
The Innovation of the Pascal Dynamic Contour Tonometer
In response to the limitations of the Goldmann tonometer, a new technology, the Pascal Dynamic Contour Tonometer, was developed. Named in honor of 17th-century physicist Blaise Pascal, known for the “Pascal Law of Pressure,” this tonometer provides a direct and accurate measurement of IOP, regardless of individual variations in corneal properties and biomechanics.
The Pascal's Approach
The Pascal tonometer operates differently from its predecessors. It has the unique ability to detect and accurately measure dynamic fluctuations in IOP linked to ocular blood flow. It samples IOP repeatedly at a rate of 100 times per second, providing a comprehensive and precise representation of the pressure changes within the eye.
Simultaneously, the Pascal tonometer records the Ocular Pulse Amplitude (OPA) and the systemic pulse rate, both vital data for glaucoma management. OPA is the difference between diastolic and systolic intraocular pressures, automatically computed by the Pascal tonometer.
Glaucoma: Essential Facts and Insights
Prevalence and Severity: Glaucoma is a leading cause of irreversible blindness if not addressed in a timely manner. This disease, often referred to as the ‘sneak thief of sight,’ progressively deteriorates vision, usually without any noticeable symptoms until substantial vision loss has taken place.
Irreversible Damage and Manageability: While there is no definitive cure for glaucoma, the progression of the disease can be slowed or halted through medications or surgical interventions, helping to prevent further vision loss. As a chronic disease, glaucoma necessitates lifelong monitoring and consistent management.
Predominant Risk Groups: It’s essential to note that certain demographics exhibit a higher susceptibility to glaucoma. Specifically, older individuals and African Americans face a significantly increased risk of developing this condition. Research indicates that African Americans are nearly three times more likely to develop open-angle glaucoma, and they tend to experience this onset at a younger age compared to Caucasians.
Other Risk Factors: Beyond age and racial background, a host of other factors can heighten the risk of glaucoma. These include a family history of glaucoma, high myopia (nearsightedness), diabetes, and systemic hypertension. Certain medications, like some sleeping pills, may also elevate the risk of glaucoma development or intensify the intraocular pressure. Therefore, it is essential to provide your eye doctor with a comprehensive overview of all medications currently being taken.
Types of Glaucoma: Apart from Open Angle Glaucoma, there are several other types, including Angle-Closure Glaucoma, Normal-Tension Glaucoma, and Secondary Glaucoma, each with its unique features and management approach.
Symptoms of Open Angle Glaucoma: Open Angle Glaucoma, the most common type of glaucoma, typically presents no symptoms and is not usually associated with pain, even when eye pressure increases. This makes regular eye examinations crucial, particularly for those individuals within higher risk groups.
Impact on Quality of Life: Due to the progressive nature of glaucoma and its capacity to impair vision, it can significantly affect a person’s quality of life, causing difficulties in daily activities like reading, driving, and recognizing faces.
Global Burden of Disease: As per the World Health Organization, glaucoma affects around 60 million people worldwide, underscoring its status as a major public health concern.
Preventive Measures: Although there’s no surefire way to prevent glaucoma, regular comprehensive eye exams can aid early detection and intervention. A healthy lifestyle, including regular exercise and a balanced diet, may also contribute to overall eye health.
With the experienced guidance of Dr. Edward Boshnick, patients receive thorough eye health assessments, including state-of-the-art glaucoma screening. His proactive approach focuses on early detection and prompt intervention to safeguard against vision loss from this silent yet dangerous disease.
Your Vision, Our Priority:
Schedule Your Consultation Now
Frequently Asked Questions
In its early stages, glaucoma often has no symptoms. As the disease progresses, you may gradually lose your peripheral (side) vision. In later stages, glaucoma can lead to tunnel vision or even total blindness.
While there’s no sure way to prevent glaucoma, regular eye exams can help detect the disease early, which is vital to prevent vision loss or slow its progress. Maintaining a healthy lifestyle—like regular exercise and a balanced diet—can also contribute to overall eye health.
Yes, glaucoma can occur in children, though it’s rare. This condition is called pediatric or childhood glaucoma. Symptoms can include excessive tearing, sensitivity to light, and a cloudy or enlarged eye.
Yes, glaucoma can run in families. If you have a parent or sibling with glaucoma, you are more likely to develop the condition. Despite this, glaucoma can still occur in people with no family history of the disease.
No, glaucoma is usually treated with eye drops and oral medication first. If these methods fail to lower the eye pressure sufficiently, then laser treatment or surgery might be considered.
Open-angle glaucoma, the most common form, involves slow clogging of the drainage canals in the eyes leading to increased eye pressure. Closed-angle glaucoma (or angle-closure glaucoma) is less common and occurs when the drainage canals get blocked suddenly, leading to a sudden rise in intraocular pressure.
Regular exercise, maintaining a healthy diet, refraining from smoking, limiting caffeine intake, and staying hydrated can help manage glaucoma. It’s important to avoid activities that might increase eye pressure, like heavy lifting. Regular follow-ups with your eye care provider are essential for managing glaucoma effectively





Schedule Your Consultation with
Dr. Boshnick
-
-
-
7800 Sw 87 Ave Suite B-270
Miami, Florida 33173
